Other Conditions
Floaters
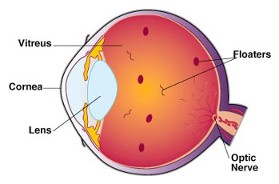
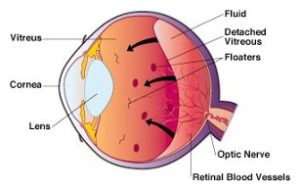
As we age, vitreous fluid, the jelly-like substance that fills the eye, degenerates. Some parts of the gel in the eye liquefy and some parts condense into particles and strands that float around the inside of the eye. They may be seen as bugs, gnats, strings, spots or spider webs that are a variety of shapes and sizes. These visually aggravating objects appear to be in the front of your vision but are actually floating within the vitreous, casting shadows on the retina. These objects could be minute amounts of blood, torn retinal tissue, inflammation or could simply be the normal aging of the gel of the eye.
These debris (floaters) are more common in nearsighted (myopic) people and those who have had cataract surgery or YAG laser surgery.
Floaters are usually nothing to worry about and usually signify a vitreous detachment, where the vitreous gel collapses away from the retina to become a freely mobile gel within the eye. However, sudden onset of many new floaters but can be a symptom of a retinal tear or detachment Therefore, it is very important to have your eyes examined with dilation by an ophthalmologist (an eye MD) if these symptoms occur. If a retinal tear is identified, it can be lasered in the office in order to prevent the tear from progressing into a retinal detachment, which could result in significant loss of vision. Floaters can be very bothersome and interfere with some visual activities. There is really no treatment or cure for vitreous floaters but they may become less noticeable over time.
Flashes
Sometimes you may have flashes along with the symptoms of floaters. Flashes may be caused by traction on the retina by the collapsing vitreous gel as it tries to separate itself from the retina This traction on the retina can stimulate the retina, causing symptoms of linear or curvilinear flashes of light off to the side of the eye, mostly noticeable in a dark room It is especially important to have your eyes dilated by an ophthalmologist if you have these symptoms as well. This needs to be evaluated immediately.
Remember, if you notice new symptoms of many new floaters and/or flashes you should be seen urgently for a dilated eye exam. If a retinal tear is identified, it is possible to laser the tear in the office before it progresses into a retinal detachment. If you see a sudden shower of floaters, a spider web, a veil or curtain that comes into your vision see your eye care specialist as quickly has possible.
Plaquenil Monitoring?

What is Plaquenil?
Plaquenil (hydroxychloroquine) is a medication that is used for rheumatologic conditions. It is most commonly used to treat rheumatoid arthritis and lupus.
Plaquenil (hydroxychloroquine) is a medication that is used for rheumatologic conditions. It is most commonly used to treat rheumatoid arthritis and lupus.
What happens when you’re taking Plaquenil?
Plaquenil is a relatively safe drug, however it can rarely cause damage to the retina. The retina is the light-sensitive tissue that lines the inside of the eye. Damage to the retina can cause vision loss. If vision loss does occur, it happens very slowly, so slowly that the patient may not notice it. Today, we have many tests that are able to be performed in the office to identify early signs of toxicity, long before a patient will notice any vision changes. Since vision loss with Plaquenil can be permanent, it is very important to identify very early signs of toxicity so the Plaquenil can be discontinued before the patient is aware of any visual problems.
Plaquenil is a relatively safe drug, however it can rarely cause damage to the retina. The retina is the light-sensitive tissue that lines the inside of the eye. Damage to the retina can cause vision loss. If vision loss does occur, it happens very slowly, so slowly that the patient may not notice it. Today, we have many tests that are able to be performed in the office to identify early signs of toxicity, long before a patient will notice any vision changes. Since vision loss with Plaquenil can be permanent, it is very important to identify very early signs of toxicity so the Plaquenil can be discontinued before the patient is aware of any visual problems.
Monitoring on Plaquenil
Patients should see an ophthalmologist as soon as they consider starting Plaquenil, and continue to see them every 6-12 months. During their visit, they should expect a dilated eye exam, as well as several tests. These tests include:
Patients should see an ophthalmologist as soon as they consider starting Plaquenil, and continue to see them every 6-12 months. During their visit, they should expect a dilated eye exam, as well as several tests. These tests include:
- Humphrey visual field: this tests your peripheral vision
- Optical coherence tomography (OCT): this takes a detailed image of the specific layers of the retina where damage can be first noticed.
- Patients should continue to see their rheumatologist and primary care physician while on Plaquenil.






